How COVID-19 Could Drive Improvements in Care Facilities (Part I)
In this first installment we assess the centrality of care facilities to the COVID-19 pandemic and outline the infection risks for residents and workers.
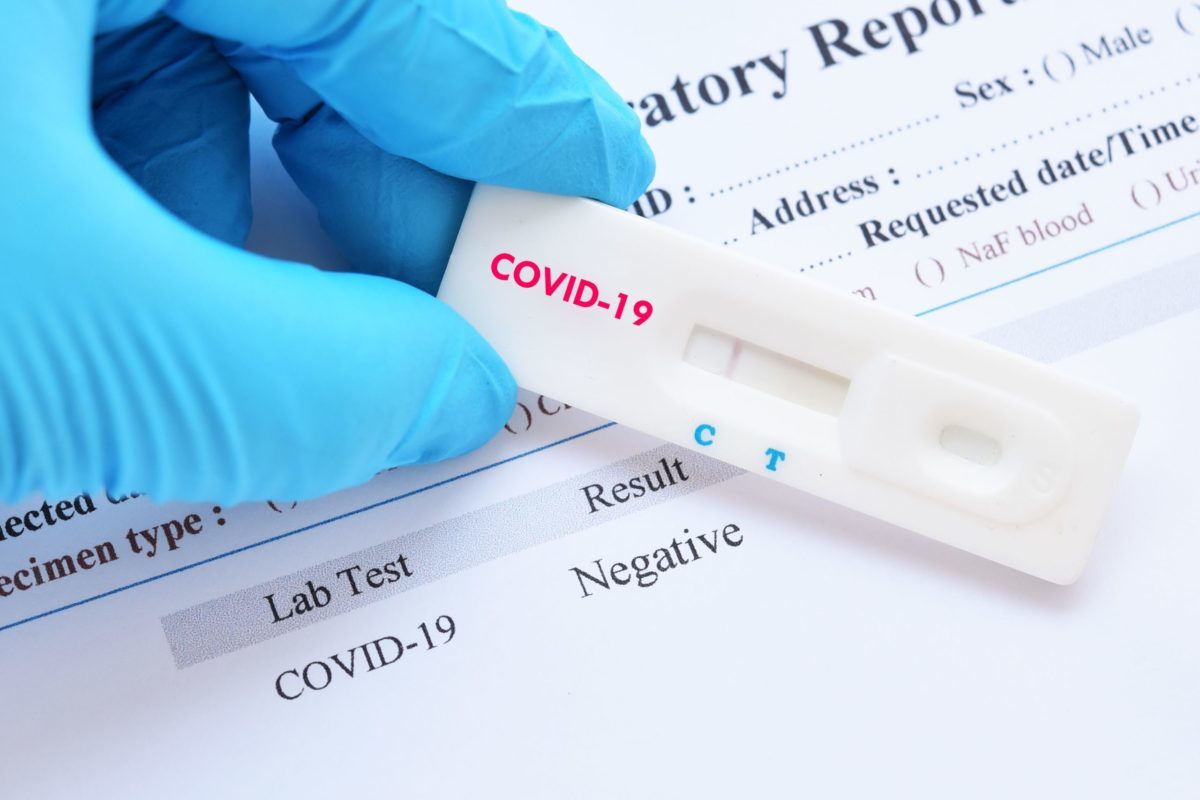
In this first installment we assess the centrality of care facilities to the COVID-19 pandemic and outline the infection risks for residents and workers.

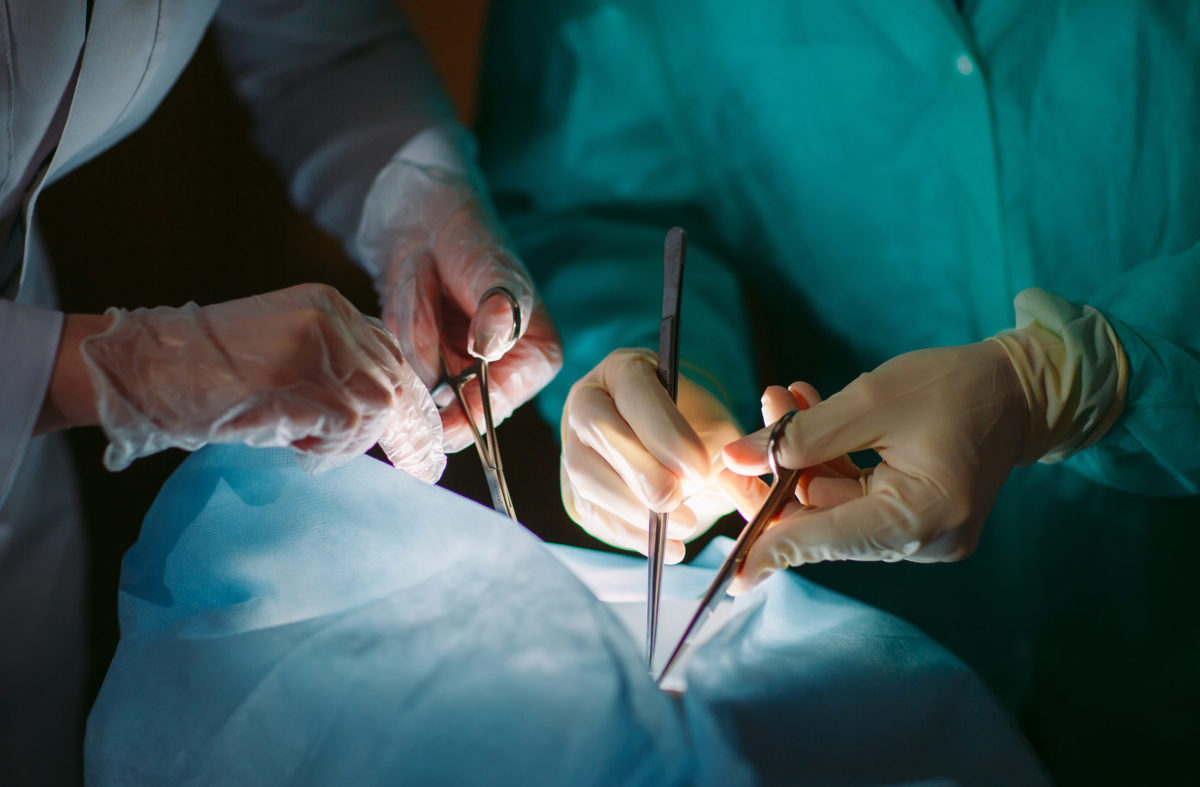
A banner year for organ transplantation in the United States became a tattered memory by April 2020, when the COVID-19 pandemic hit.
Beyond specific violations of rights, it is important to note that the executive used the COVID-19 crisis to limit the work of other branches of government.

Like many other countries, different levels of government in Canada have adopted a wide range of measures in response to COVID-19.

A state of sanitary emergency was declared for two months in order to allow the authorities “to deal with the major health threat” posed by COVID-19.

Coronavirus misinformation is beating truth to the punch. This “infodemic” anchors readers to its core messages and makes dislodging falsehoods difficult.
With the amendment, power that had previously belonged to regional commissions was transferred and centralized to the Health Minister.

On March 16th, Prime Minister Mark Rutte announced a range of measures aimed at “maximum control,” but not “maximum containment” of the virus.

As of May 22nd, new infections have reduced to a trickle – there are often zero new cases per day, after weeks of being in the single digits.

The measures taken in the U.K. to respond to the pandemic have been described as “almost certainly the most severe restrictions on liberty ever imposed.”
