Addressing Health Inequities in End-of-Life Care in the Era of COVID-19
Inequities in end-of-life care have been exacerbated by the COVID-19 pandemic, but have yet to receive the same attention as other health disparities.

Inequities in end-of-life care have been exacerbated by the COVID-19 pandemic, but have yet to receive the same attention as other health disparities.

While telehealth may be a panacea for access to healthcare, particularly in COVID times, we should be concerned that patients of color may be left behind.

Medical neocolonialism does not exist in a vacuum. It is tied to the presumed expendability of Black life.
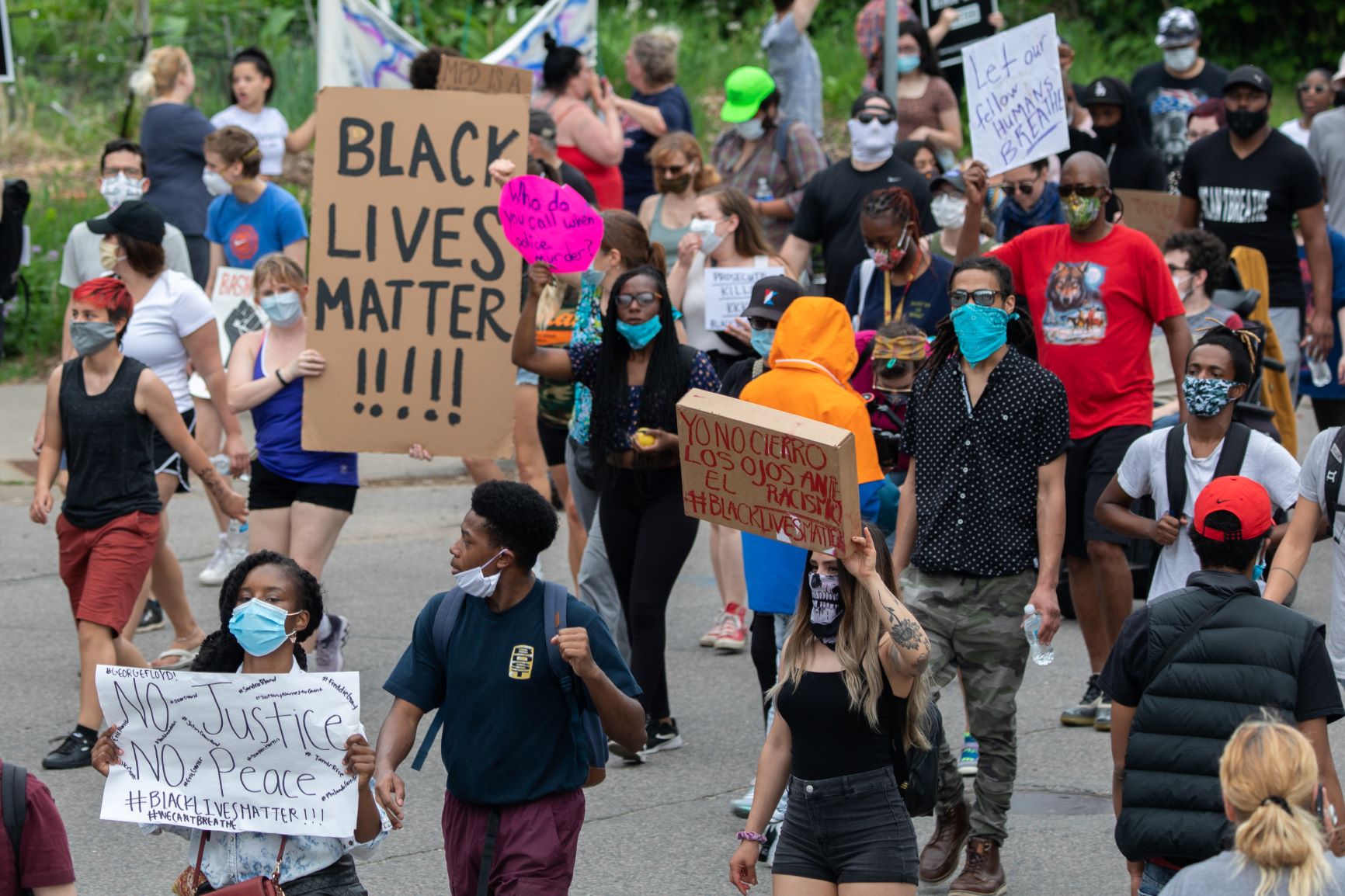
The COVID-19 pandemic has highlighted the tradeoffs at stake for Black, Indigenous, and people of color (BIPOC) seeking reliable health advice.

Too often, policies and practices in schools that create and compound health inequities are narrated as falling outside health law and policy.

During the COVID-19 pandemic, instead of trying to extinguish racist attitudes, the Trump administration has spearheaded ways to “other” Asian Americans.

Social, economic, and environmental factors account for the vast majority of health outcomes. And housing encompasses many of these factors.
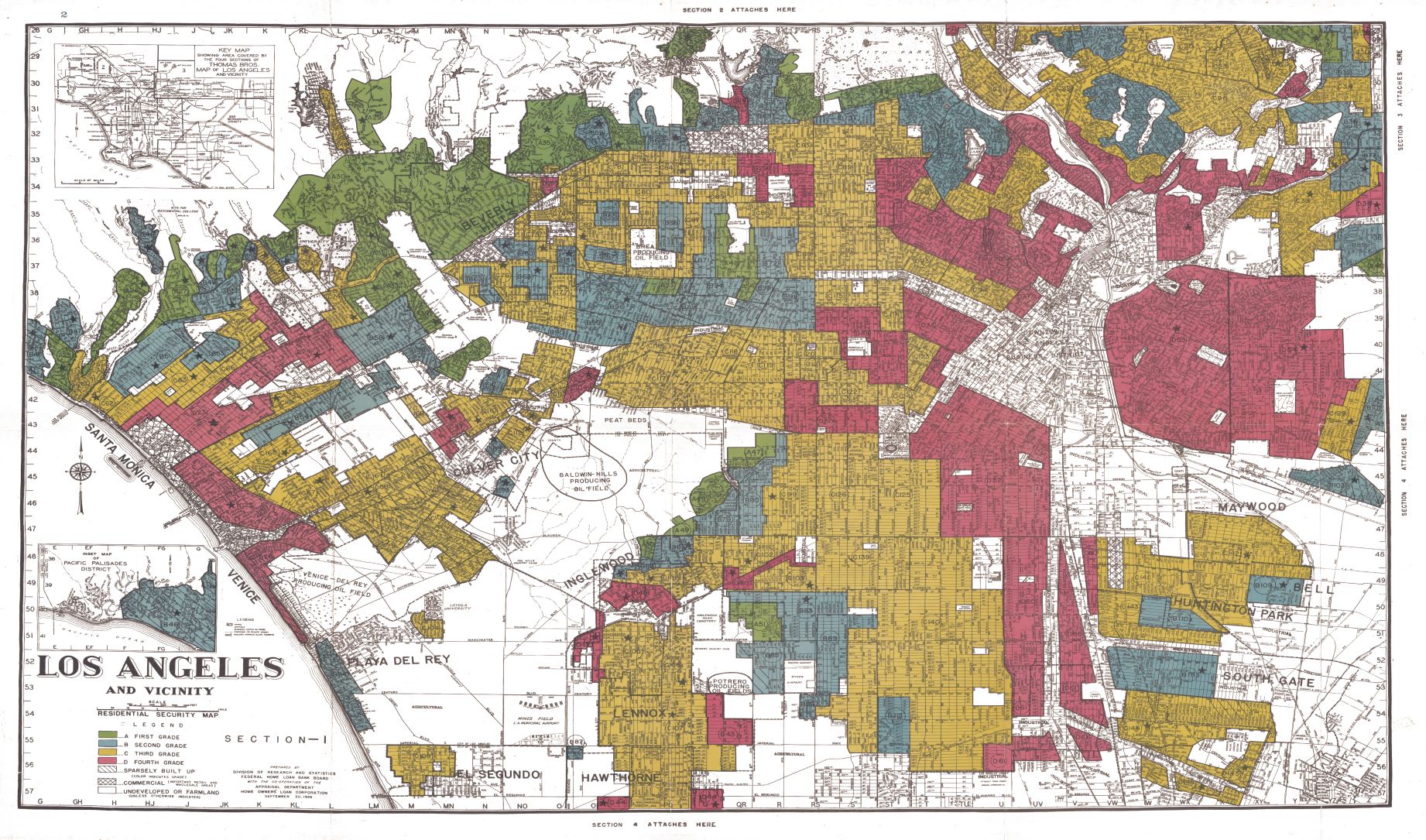
Debates exist over whether structural racism is a social determinant of health, and whether dismantling it is within the scope of public health law.

Considering the cross-cutting nature of racism as a social determinant of health, medical-legal partnerships can and should address it directly.

Scholarship on the social determinants of health is missing an account of how communities change the legal environments that produce poor health outcomes.